Keloids can be stubborn. Many individuals look for ways to control them. Fortunately, surgery isn’t always required. Effective non-surgical treatments exist. Knowing these options is essential.
Managing keloids can be discouraging. These prominent scars frequently extend beyond the original injury. They often cause discomfort and alter appearance. Selecting effective treatments for keloids is vital for many.
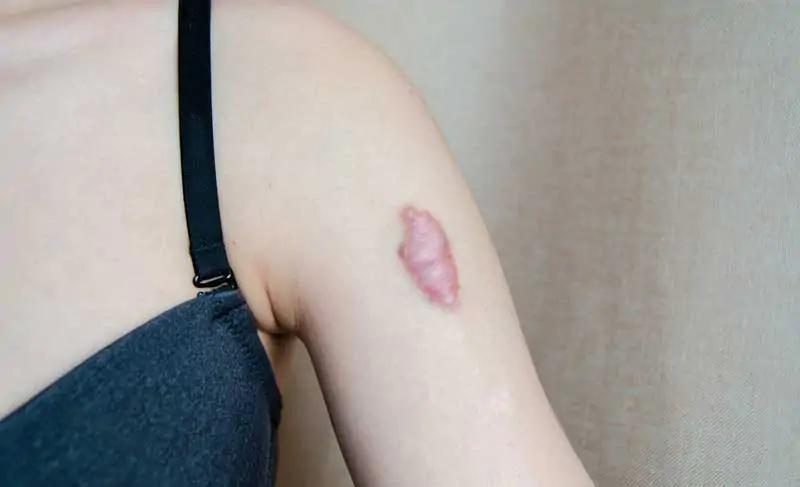
Keloids differ from ordinary scars. They are thick, fibrous masses arising after skin trauma, such as cuts, burns, or piercings. Genetics strongly influences their formation.
Individuals with darker skin tones, including those of African, Asian, and Hispanic descent, may be more prone. Keloids affect millions and impact the quality of life.
Many individuals fear surgical removal due to recurrence risk. Keloids sometimes return larger than before. As a result, non-surgical options are often favored. These approaches offer a safer alternative.
This guide examines diverse methods. We will review validated strategies intended to minimize keloid size and improve appearance. We will also cover prevention of recurrence, drawing on reliable medical evidence.
Understanding Keloids: What Are They?
A keloid is a type of raised scar. It appears after skin damage. Unlike normal scars, keloids grow excessively. They extend beyond the original wound margins. This makes them distinctive.
Formation and Characteristics
Keloids form when the skin heals. Fibroblasts produce too much collagen. This excessive collagen builds up. It creates a firm, rubbery lesion. They can be pink, red, or skin-colored.
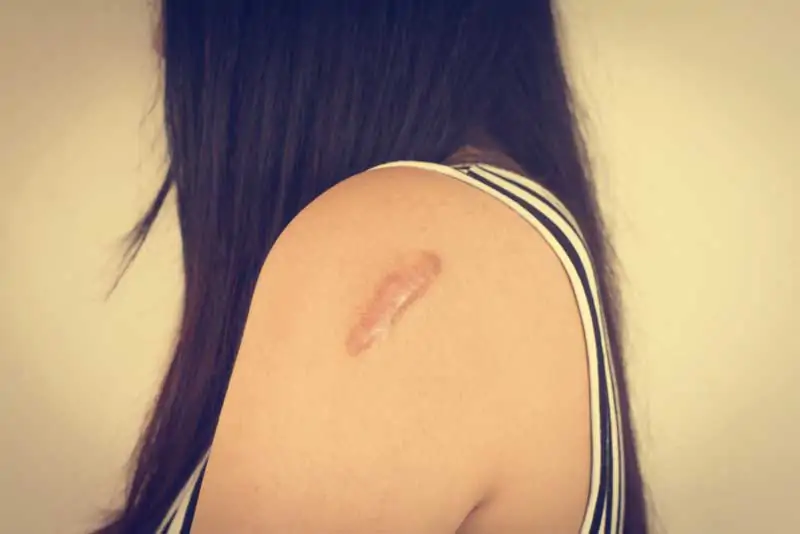
Common sites include the chest, shoulders, and ears. They also appear on the back and neck. Keloids can cause itching or pain. They might also feel tender to the touch. Their size varies greatly.
Who Is at Risk?
Keloid risk factors are largely genetic. Family history heightens susceptibility. Age is relevant; young adults aged 10–30 are most vulnerable. Skin tone is a critical element. Studies indicate keloids may be more prevalent among people of African descent, yet prevalence varies across populations.
Non-Surgical Keloid Removal Methods
Several proven non-surgical treatments are available. These aim to flatten, soften, and diminish keloids. Success rates differ per individual. Consistent application is essential for optimal results.
1. Corticosteroid Injections
Intralesional corticosteroid injections are a primary treatment. Triamcinolone acetonide is a common choice. It reduces inflammation. It also breaks down collagen production. Injections are given directly into the keloid.
Treatments occur every 3-4 weeks. Multiple sessions are often needed. This method helps flatten keloids. It also alleviates symptoms like itching. Around 50-100% of keloids respond well. However, recurrence rates vary. Some studies show a recurrence rate of 9-50% in cases.
2. Silicone Sheets and Gels
Silicone products are often recommended. They form a protective barrier that hydrates skin and modulates collagen formation. Silicone sheets require extended daily wear; gels are applied twice daily.
Consistency is essential. Apply for 3-6 months. Silicone markedly improves the appearance of keloids; it flattens and softens scars. Many patients consider this method comfortable and non-invasive.
3. Pressure Therapy
Pressure garments or clips apply constant pressure. This reduces blood flow to the keloid. Decreased blood supply inhibits collagen growth. It helps to flatten the scar over time.
Pressure therapy prevents keloid recurrence post-surgery but can also be used alone. Devices are worn for months, sometimes up to a year. Adherence is vital for success.
4. Cryotherapy
Cryotherapy involves freezing the keloid. Liquid nitrogen is typically used. This causes cell death. The keloid eventually shrinks. It is particularly effective for smaller keloids.
Multiple cryotherapy sessions are needed, spaced a few weeks apart. Combined with injections, outcomes improve, with response rates of 60-80%.
5. Laser Therapy
Various lasers can treat keloids. Pulsed dye lasers (PDL) target blood vessels. They reduce redness and flatten the scar. Fractional CO2 lasers improve texture. They also enhance drug penetration.
Laser therapy requires multiple sessions and can be expensive, but offers significant cosmetic improvement—especially when combined with other treatments for maximum efficacy.
6. Imiquimod Cream
Imiquimod is a topical immune response modifier that stimulates interferon production, helping reduce collagen and prevent recurrence after treatment.
Often used post-excision to reduce keloid regrowth, Imiquimod can also be used alone, though its effectiveness is under research, and it may cause skin irritation.
7. 5-Fluorouracil (5-FU) Injections
5-FU, an anti-cancer drug, inhibits fibroblast proliferation and reduces collagen when injected into keloids. It is often combined with corticosteroids to flatten and soften keloids.
This combination yields better results but can cause pain and hyperpigmentation. Regular injections are needed for optimal results, and the method is gaining popularity.
8. Radiation Therapy
Radiation therapy targets keloid-forming cells with high-energy rays to inhibit growth, typically used for recurrent keloids after surgery.
Often given shortly after surgery, radiation therapy significantly reduces recurrence, with studies showing rates as low as 10-20% when combined with surgery.
Expert Insights on Keloid Management
“The key to managing keloids effectively lies in a multi-modal approach. No single treatment works for everyone. Combining therapies, such as corticosteroid injections with silicone sheeting, often yields the best results. Patient adherence is paramount for long-term success.” – Dr. Eleanor Vance, Dermatologist, London, UK.
“Early intervention is crucial for keloids. The sooner treatment begins, the better the prognosis. Even small keloids can grow significantly if left untreated. Always consult with a specialist to determine the most appropriate treatment plan for your specific situation.” – Prof. Jean-Pierre Dubois, Plastic Surgeon, Paris, France.
Preventing Keloid Formation
Prevention is always better than a cure. Especially for those prone to keloids. Taking proactive steps can minimize risk.
Key Prevention Strategies
- Avoid Unnecessary Skin Trauma: Be cautious with piercings, tattoos, and cosmetic surgeries.
- Proper Wound Care: Keep wounds clean and moist. Use petroleum jelly or silicone gels.
- Pressure Dressings: Apply pressure immediately after injury. This helps prevent excessive scarring.
- Silicone Products: Use silicone sheets or gels on healing wounds. Start early for best results.
- Sun Protection: Protect new scars from direct sunlight. UV rays can darken keloids.
- Consult a Dermatologist: If you have a history of keloids, seek expert advice before any skin procedure.
Choosing the Right Treatment for You
The optimal keloid treatment depends on several factors, including keloid size, location, and your medical history. Your dermatologist will evaluate your condition and recommend a personalized treatment plan to achieve the best possible results.
For Australians residing in Bali, accessing specialized medical care is important. Keloid treatment is offered at various dermatology and aesthetic clinics. Patients should consult a board-certified dermatologist or plastic surgeon. Bali Sudirman Medical Center provides comprehensive, non-surgical keloid treatments and personalized care, with modern facilities and experienced professionals who understand the needs of international patients.
Consider a consultation at Bali Sudirman Medical Center, where our team will guide you through your options and support your informed decision-making. Achieving smoother, healthier skin is within reach. We are committed to providing effective, humane, and unique solutions that enhance your health journey.
Conclusion: A Path to Smoother Skin
Living with keloids is challenging, but many non-surgical options offer hope to reduce their appearance and alleviate symptoms.
Always seek professional medical advice. A qualified dermatologist or plastic surgeon will create a personalized plan. Consistency in treatment ensures the best outcomes.
Do you have questions about keloid treatment or need personalized advice? Schedule a consultation at Bali Sudirman Medical Center—our team is ready to assist you. Explore our comprehensive aesthetic services at BSMC Aesthetic Services. To reserve your visit, please visit the BSMC Reservation Page. Take the first step toward clearer, healthier skin today.
Frequently Asked Questions (FAQ)
Q: Can keloids disappear completely without surgery?
A: Total involution is uncommon; treatment usually aims to flatten, soften, and improve color and symptoms.
Q: How long does non-surgical keloid treatment take?
A: Treatment duration varies. It depends on the method and the keloid size. It can range from a few weeks to several months. Patience and consistency are crucial.
Q: Are non-surgical treatments painful?
A: Some treatments involve mild discomfort. Corticosteroid injections might sting. Laser therapy can cause a warm sensation. Topical anesthetics can help manage pain.
Q: Can keloids grow back after non-surgical treatment?
A: Yes, recurrence is possible. Even with non-surgical methods. Ongoing management and preventive measures are important. This helps maintain results over time.
Q: What is the most effective non-surgical treatment for keloids?
A: No single treatment is universally the most effective; often, a combination of therapies tailored to the keloid’s size, location, and patient factors works best. Combination therapies (e.g., steroid + 5-FU + laser) are increasingly used to improve response and reduce recurrence.
Q: Where can I get keloid treatment in Bali?
A: Bali Sudirman Medical Center offers various keloid treatments. They provide expert care and modern facilities. This is ideal for those living in or visiting Bali.
For more information or to book an appointment, visit our reservation page today!